 
It is crucial to conduct research on the virus’s defense mechanisms, especially how certain T cells interact with SARS-CoV-2, in addition to research on antibodies in the disease, is essential to fill the current knowledge gap to improve vaccine design ( 16). All these factors can cause widespread lung tissue damage and subsequent thrombotic events ( 14, 15). Acute respiratory distress syndrome (ARDS) and multiple organ failure are its hallmarks, while lymphocyte depletion, cytokine storm, and delayed and defective interferon (IFN) response are all present. There are signs that the immunological dysregulation caused by SARS-CoV-2 contributes more to the intensity of the disease than the virus itself. Furthermore, many peptides derived from SARS-CoV-2, such as those from the M protein, induced specific memory T cell responses, as well as IFN-gamma responses, in recovered patients ( 12, 13). Although neutralizing antibodies from exposure to CoV cannot prevent infection by a variant or SARS-CoV-2, the disease can have a milder course ( 9, 11). Most infected people produce IgM, IgG, and IgA antibodies against the Spike protein and its receptor-binding domain (RBD) in response to SARS-CoV-2. Therefore, seroconversion of the disease by IgM, although it can start on the fifth day of symptom onset, due to individual variability of the immune response, is best measured on the 10 th day of symptom and IgG on the 14 th day ( 10).īoth protective immunity and protection against reinfection are provided by natural SARS-CoV-2 infection. In patients with COVID-19, there is an incubation time of 4 to 7 days before the onset of symptoms and an additional 7 to 10 days before individual progress to severe illness. However, in addition to being more specific, compared to antibodies against nucleocapsid proteins, antibodies against RBD emerge sooner during the infection ( 9). However, it is proposed that the exacerbated inflammatory immune response against SARS-CoV-2 is related to the disease severity ( 7).Įach SARS-CoV-2 protein can initiate an immunological response that results in the generation of antibodies, and it has been shown that protein S and protein N are antigens that result in the development of neutralizing antibodies when present in high quantities ( 8). The adaptive response is capable of producing immune memory and control of viral infection in a way that its understanding in COVID-19 is essential. The adaptive system is made up of antibody-producing B cells, CD4+ T cells with various adjuvant and effector mechanisms, and CD8+ T cells with cytotoxic potential. Although innate and adaptive immune responses are interconnected and play a joint role, each of them has specialized cells with distinct functions. 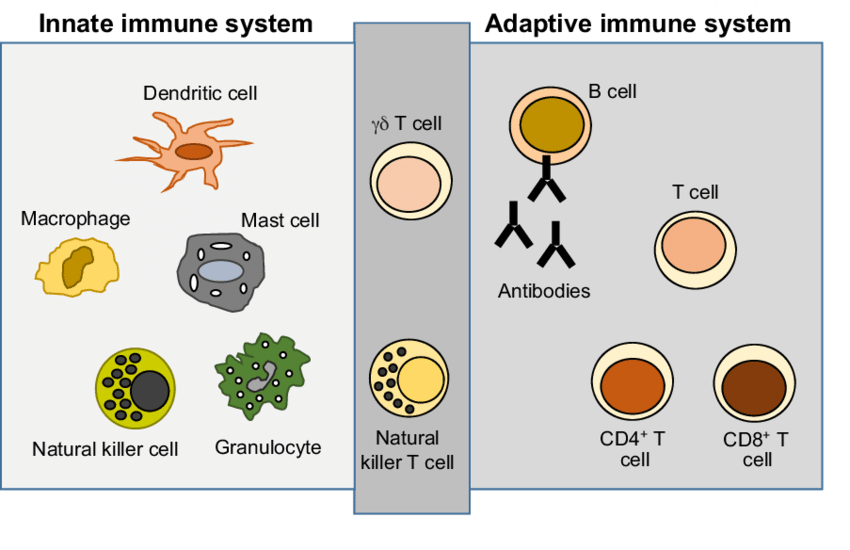
The human immune system is divided into innate and adaptive. Clinically, patients with COVID-19 can be classified as mild (no lung involvement), moderate (with respiratory symptoms), severe (greater lung involvement, with uncontrolled systemic inflammation) and critical (requirement for mechanical ventilation and signs of septic shock) ( 6). COVID-19, which arises from a Betacoronavirus of zoonotic origin that was first reported in Wuhan, China, has resulted in high rates of morbidity and mortality worldwide ( 2).Ĭurrently, the main antigen of the virus is the SARS-CoV-2 S (Spike) protein, which can bind the virus to the human angiotensin converting enzyme 2 receptor (ACE2) through the receptor binding domain (RBD) and thus allow its entry into the cell ( 3– 5). The 2019 coronavirus disease pandemic (COVID-19) began its occurrence around March 2020 according to the World Health Organization (WHO) through a novel coronavirus (CoV) that causes severe acute respiratory syndrome (SARS) ( 1). Among the antibodies produced by SARS-CoV-2, Immunoglobulin (Ig) A stood out due to its potent release associated with a more severe clinical form. Some CD8+ T lymphocyte markers are associated with the severity of the disease, such as human leukocyte antigen (HLA-DR) and programmed cell death protein 1 (PD-1). These cells are responsible for the secretion of cytokines, including interleukin (IL) - 6, IL-4, IL-10, IL-7, IL-22, IL-21, IL-15, IL-1α, IL-23, IL-5, IL-13, IL-2, IL-17, tumor necrosis factor alpha (TNF-α), CXC motivating ligand (CXCL) 8, CXCL9 and tumor growth factor beta (TGF-β), with the abovementioned first 8 inflammatory mediators related to clinical benefits, while the others to a poor prognosis. The predominant subpopulations of T helper lymphocytes (Th) in critically ill patients are Th1, Th2, Th17 (without their main characteristics) and regulatory T cells (Treg), while in mild cases there is an influx of Th1, Th2, Th17 and follicular T helper cells (Tfh). CD4+ T cells were the most resolutive in the health-disease process compared with B cells and CD8+ T lymphocytes. Fifty-six articles were finalized for this review.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
